Are Swellings Around the Cornea Common After Cataract Surgery?
It’s common to have corneal swelling or edema during the first few days of cataract surgery, which may lead to some temporary foggy vision.
Generally, swelling after cataract surgery will go away and vision will be clear in a few days, however, rare corneal swelling may not improve if the cornea is weak, like in Fuchs’ Dystrophy, keratoconus, or if the cataract is very dense and hard to remove.
If a cataract surgery patient’s cornea is swollen for an extended period of time, it might take up to three months to establish if the swelling will clear on its own, however, when it is mild and not affecting the vision, no treatment is necessary.
Eye drops can be used to lower the swelling of mild morning blurred vision; however, if it doesn’t get better over time, a corneal transplant might be required for proper vision restoration.
Causes of Corneal Edema
Corneal edema can be caused by a malfunctioning of the inner corneal layer. Normally, endothelial cells pump out fluid, creating a clear vision and healthy eyes.
Illness or injuries can lead to a breakdown in the endothelium function, which then causes fluid build-up and the cornea swells. This occurrence is associated with several other health issues.
Fuch’s endothelial dystrophy, which is caused by genetic factors that lead to the gradual loss of cells in the endothelium, is a common occurrence, commonly evidenced in those over 50 years of age and more prevalent in women than men.
Other things that could help trigger Fuch’s include:
- Some medications
- Eye surgery
- Contact lenses
- Other medical conditions like herpes
Other possible causes of corneal edema include:
- Injury to your eye from a blow or a puncture
- Inflammation due to problems like rheumatoid arthritis or specific eye issues like iritis or keratitis
- Poisonous substances that inflame, irritate, or damage parts of your eye
Symptoms of Corneal Edema
One of the initial notes you might observe is vision impairment. Typically, it could appear worst in the morning and may improve as the day goes on.
You might also have:
- A scratchy feeling in your eye
- Pain or tenderness when you touch your eye
- Eye pain or discomfort in light
- Hazy circles, or “halos,” around lights
- In rare or serious cases, painful blisters in your eye
Diagnosis of Corneal Edema
After discussing your medical background and any symptoms you may have with your doctor, they will inspect your eyes. If there are signs of corneal edema, your doctor may:
- Look for scars or cloudiness on your cornea
- Use magnifiers like a slit lamp or an ophthalmoscope to see details of your eye
- They may measure the thickness of your cornea using a pachymeter and an ultrasound to get a better view of your eye
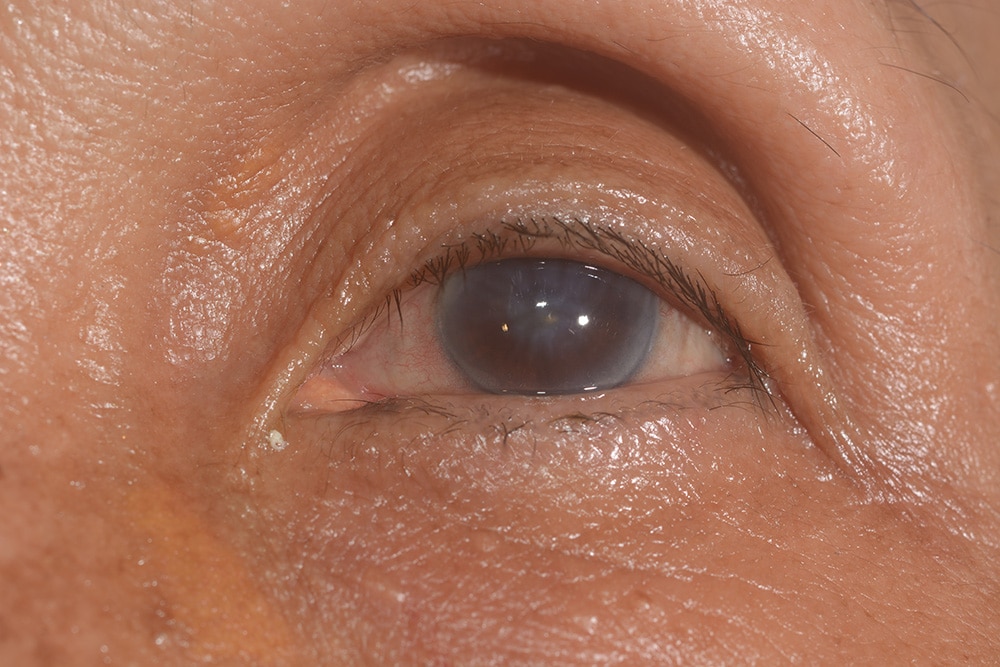
Treatment options for corneal edema
If the corneal edema is not severe, treatment may not be necessary. However, to provide some temporary relief from swelling in the eye, your eye doctor might suggest you use concentrated salt and water drops or ointment.
To reduce the swelling overnight, ask your doctor if you can use a hair dryer in the morning to evaporate the excess tears. Make sure to hold the dryer at a distance to prevent any injury.
If the swelling is so severe that it harms your sight, you may need surgery. The procedure consists of replacing either the whole cornea or just its endothelial layer with healthy corneal tissue from a donor. Other treatments for corneal edema include:
Penetrating keratoplasty (PK or PKP)
In order to replace the unhealthy tissue in your cornea with healthy donor tissue, the surgeon will remove all layers of your cornea and secure the new tissue with sutures.
As the graft may be misshapen, wearing glasses or contact lenses after the surgery may be necessary for clear vision.
Also, risks such as glaucoma, damage to the eye lens, bleeding, or graft rejection are present in PKP surgery.
Descemet’s stripping endothelial keratoplasty (DSEK)
Compared to PK, the procedure for this is faster and the recovery time is shorter since it only replaces the damaged endothelium layer of your cornea – not the entire thing.
This procedure replaces a thin layer of tissue inside the eye known as the “Descemet membrane” which helps prevent fluid from building up, thus preventing or limiting edema. DSEK is often an ideal option for those with corneal swelling due to cataract surgery since its success rate is high and it requires significantly less recovery time than other procedures.
Healing time and recovery
The length of your recovery period depends on how severe your corneal edema is, and the treatment plan you follow, that is why minor corneal edema might not even cause any symptoms or may not require any treatment.
After a corneal transplant operation, it may take up to one year before restoring your vision completely. In addition, irregularly shaped tissue could require you to wear glasses to attain the clear vision.
The healing process is quicker when you opt for a DSEK procedure, which just involves the removal of part of the cornea.
Prevention of Corneal Edema
Prevention of Corneal Edema after cataract surgery starts at the pre-operative stage. Patients should inform their eye surgeon about any previous corneal issues or allergies, as well as any medications or procedures that could affect the healing process.
During surgery, your eye surgeon should use special equipment and techniques to prevent damage to the cornea, such as using a special microscope to guide the removal of the lens capsule with accuracy and precision. Post-operatively, cataract surgery Hawaii patients should follow their eye doctor’s instructions carefully in order to ensure proper healing and reduce the risk of edema development.
Ready for a consultation?
If you are looking for treatment options and want state-of-the-art laser eye surgery to cure your blurry vision, the cataract treatment specialists at EyeSight Hawaii in Honolulu, HI, and Maui, HI has the experience and knowledge to help. Make an appointment online or call our office to schedule a consultation today!

